A6 - Combining real-time brain imaging with neurofeedback to modulate the desire for food
This project has been funded by the DFG from 2013 to 2016.
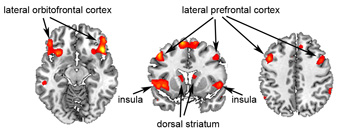
Growing evidence suggests that obesity is linked to an imbalance between the brain’s homeostatic, hedonic, and cognitive control systems. Given virtually unlimited access to high-caloric food, it is important to keep control over hedonic systems to avoid eating beyond energy demand. In a recent study, we investigated how the brain allows lean individuals to consciously regulate/control the hedonic system and hence the desire for tasty but unhealthy food (Hollmann et al., 2011). We identified the brain’s valuation system in combination with prefrontal cognitive control areas to contribute to active reappraisal of unhealthy food. An insufficient cognitive control capacity of these brain systems represents one crucial mechanism in the development of obesity. Here, we aim to combine real-time functional magnetic resonance imaging (rt-fMRI) with neurofeedback to train obese subjects on strengthening cognitive control over the hedonic brain system and hence overeating behavior. We acquire hemodynamic brain responses from obese subjects in real-time to continuously monitor current brain states. The difference between this state and a state of optimized cognitive control will be translated into a single signal and visually backprojected to the subject on-line (i.e. neurofeedback). With the following presentations subjects will be trained to continuously adapt their current brain state to a state of optimized cognitive control. We aim at comparing two different training approaches: training (i) on one’s own brain pattern of optimized control, or (ii) on brain patterns of lean subjects. We hypothesize that with ongoing neurofeedback training, subjects progressively learn to use the most advantageous strategy in order to gain control over desire for unhealthy food. Strengthening cognitive control over eating through neurofeedback represents a promising approach for the development of new treatment strategies in obesity.
Figure 1. Shown are brain regions that allow lean individuals to consciously regulate/control the hedonic system and hence the desire for tasty but unhealthy food (see also Hollmann et al., 2011).
Rullmann M, Preusser S, Poppitz S, Heba S, Gousias K, Hoyer J, Schütz T, Dietrich A, Müller K, Hankir MK, Pleger B., Adiposity Related Brain Plasticity Induced by Bariatric Surgery., Front Hum Neurosci. 2019 Aug 27;13:290.
Hankir MK, Rullmann M, Seyfried F, Preusser S, Poppitz S, Heba S, Gousias K, Hoyer J, Schütz T, Dietrich A, Müller K, Pleger B. Roux-en-Y gastric bypass surgery progressively alters radiologic measures of hypothalamic inflammation in obese patients. JCI Insight. 2019 Aug 29. pii: 131329.
Kumar S, Grundeis F, Brand C, Hwang HJ, Mehnert J, Pleger B. Satiety-induced enhanced neuronal activity in the frontal operculum relates to the desire for food in the obese female brain. Exp Brain Res. 2018 Jun 22.
Rullmann M, Preusser S, Poppitz S, Heba S, Hoyer J, Schütz T, Dietrich A, Müller K, Pleger B. Gastric-bypass surgery induced widespread neural plasticity of the obese human brain. Neuroimage. 2017; Epub ahead of print.
Hellrung L, Dietrich A, Hollmann M, Pleger B, Kalberlah C, Roggenhofer E, Villringer A, Horstmann A. Intermittent compared to continuous real-time fMRI neurofeedback boosts control over amygdala activation. NeuroImage. 2017;166:198-208.
Grundeis F, Brand C, Kumar S, Rullmann M, Mehnert J, Pleger B. Non-invasive prefrontal/frontal brain stimulation is not effective in modulating food reappraisal abilities or calorie consumption in obese females. Front Neurosci. 2017;11/334.
Weise CM, Piaggi P, Reinhardt M, Chen K, Savage CR, Krakoff J, Pleger B. The obese brain as a heritable phenotype - A combined morphometry and twin study. Int J Obes (Lond). 2017;41:458-66.
Kumar S, Grundeis F, Brand C, Hwang HJ, Mehnert J, Pleger B. Differences in insula and pre-/frontal responses during reappraisal of food in lean and obese humans. Front Hum Neurosci. 2016;10:233.
Melasch JT, Rullmann M, Hilbert A, Luthardt J, Becker GA, Patt M, Stumvoll M, Blüher M, Villringer A, Arelin K, Meyer PM, Bresch A, Sabri O, Hesse S, Pleger B. Sex differences in serotonin-hypothalamic connections underpin a diminished sense of emotional well-being with increasing body weight. Int J Obes (Lond). 2016;40:1268-77.
Melasch J, Rullmann M, Hilbert A, Luthardt J, Becker GA, Patt M, Villringer A, Arelin K, Meyer PM, Lobsien D, Ding Y-S, Müller K, Sabri O, Hesse S, Pleger B. The central nervours norepinephrine network links a diminished sense of emotional well-being to an increased body weight. Int J Obes. 2016;40:779-87.
Mueller K, Möller HE, Horstmann A, Busse-Voigt FP, Lepsien J, Blüher M, Stumvoll M, Villringer A, Pleger B. Physical exercise in overweight to obese individuals induces metabolic- and neurotrophic-related structural brain plasticity. Front Hum Neurosci. 2015;9:372.
Mueller K, Horstmann A, Möller HE, Anwander A, Lepsien J, Schroeter ML, Villringer A, Pleger B. Obesity associated cerebral gray and white matter alterations are interrelated in the female brain. PLoS One. 2014;9:e114206.
Horstmann A, Kovacs P, Kabisch S, Boettcher Y, Schloegl H, Toenjes A, Stumvoll M, Pleger B*, Villringer A*. Common genetic variation near MC4R has a sex-specific impact on human brain structure and brain behavior. PLoS One. 2013;8:e74362.
Schlögl H, Kabisch S, Horstmann A, Lohmann G, Müller K, Lepsien J, Busse-Voigt F, Kratzsch J, Pleger B, Villringer A, Stumvoll M. Exenatide-induced reduction in energy intake is associated with increase in hypothalamic connectivity. Diab Care. 2013;36:1933-40.
Hollmann M, Hellrung L, Pleger B, Schlögl H, Kabisch S, Stumvoll M, Villringer A, Horstmann A. Neural Correlates of the Volitional Regulation of the Desire for Food. Int J Obes. 2012;36:648-55.
Müller K, Anwander A, Möller HE, Horstmann A, Lepsien J, Busse FP, Mohammadi S, Schröter ML, Stumvoll M, Villringer A, Pleger B. Sex-dependent influences of obesity on cerebral white matter investigated by diffusion-tensor imaging. Plos One. 2011;6:e18544.
Horstmann A, Busse FP, Mathar D, Müller K, Lepsien J, Schlögl H, Kabisch, S, Kratzsch J, Neumann J, Stumvoll M, Villringer A, Pleger B. Obesity-related differences between women and men in brain structure and goal-directed behavior. Front Hum Neurosci. 2011;5:58.
PROJECT TEAM
PD Dr. Burkhard Pleger
BG University Clinic Bergmannsheil
Ruhr-University Bochum, Department of Neurology and
Max Planck Institute for Cognition and Brain Sciences
Department of Neurology
Bürkle-de-la-Camp-Platz 1
44789 Bochum
e-mail: burkhard.pleger@bergmannsheil.de
Phone: 02341 / 302-3551